Healthy building strategies that improve air quality and clean surfaces should be incorporated as part of a layered defense against COVID-19. For improving indoor air quality in the classroom, we recommend prioritizing control strategies — ventilation, filtration, supplemental air cleaning — and targeting a combined 4-6 air changes per hour (ACH) for classrooms through any combination of these approaches. Other spaces in schools such as gyms, auditoriums, kitchens, and nurses’ offices may require different targets for the combined clean air change rates.
ACH can be calculated by adding the total amount of “clean” air entering the room and dividing it by the room volume. The “clean” air in a classroom can be calculated as the sum of the ACH from ventilation (e.g. outdoor air supplied by a mechanical system or open windows), from filtration of recirculated air by a mechanical heating, ventilation, and air conditioning (HVAC) system (accounting for the efficiency level of the filters in the system), and from air cleaning provided by a portable air cleaner with a HEPA filter.
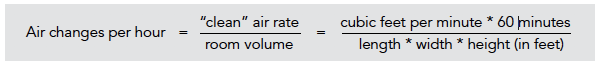

Additional information on how to assess ventilation in classrooms and calculate the total, combined ACH in a classroom can be found in this 5-step guide to checking ventilation rates in classrooms: https://schools.forhealth.org/ventilation-guide
A simple tool for helping select an appropriate portable air cleaner for a classroom and for understanding the air change per hour calculation can be found here: https://tinyurl.com/portableaircleanertool
For more technical information on portable air cleaners and how to select portable air cleaners, please read our white paper, “Portable Air Cleaners: Selection and Application Considerations for COVID-19 Risk Reduction”: https://schools.forhealth.org/wp-content/uploads/sites/19/2020/08/Harvard-Healthy-Buildings-Program-Portable-Air-Cleaners
System performance should be verified regularly. For more detailed and technical guidance, we recommend reviewing the materials produced by the ASHRAE Epidemic Task Force. Schools should work with facilities managers and outside professionals to tailor these recommendations for their unique building systems.
SARS-CoV-2 present in the coughs, sneezes, and exhaled breath of an infectious person can be transported in the air to disperse throughout a room and can remain aloft for hours. This long-range airborne virus can infect even people who haven’t had close contact with the infectious person if they inhale a sufficient amount of virus. Bringing fresh outdoor air into a room can dilute and/or displace any present airborne virus, which thus reduces the probability that someone breathes enough infectious aerosol to become infected. As an ideal, holding class outdoors provides the freshest air and most effective dilution of any infectious airborne SARS-CoV-2.
Buildings should eliminate or minimize air recirculation (thus maximizing fresh outdoor air) to the extent possible during this period.
As the next best solution, mechanical ventilation systems in buildings can forcibly bring outdoor air inside and then distribute that fresh air to different areas of the building. In some HVAC systems, some fraction of the indoor air is recirculated and mixed with the outdoor air coming in to save on cooling and heating energy costs. However, during a pandemic, when long-range airborne viral transmission can occur, air recirculation can lead to a buildup of airborne viral particles indoors and also potentially spread the virus to other areas of the building. Therefore, buildings with HVAC systems that mix the fresh outdoor air with recirculated air should maximize fresh outdoor air to the extent possible during this period. These types of buildings should also install MERV 13 air filters or higher in their HVAC systems (see next section for details). In addition, buildings should not shut off or reduce their mechanical ventilation during beforeschool or after-school hours when there still may be people in the building, including students, staff, and custodians during any student programs, cleaning times, teacher class preparation, sports (e.g., if students are returning to lockers), or other activities. Finally, mechanically ventilated schools should evaluate any potential contaminant source near the outdoor air intake duct. For example, the outdoor air inlet should not be located too close to the exhaust air outlet or contaminated indoor air that is exhausted out of the building could re-enter (refer to local building codes on minimum required distance, generally 10 feet).
Devices that simply recirculate the same indoor air without filtering it or replacing it with fresh air are not helpful in reducing any airborne virus present in the room
Schools that do not have mechanical ventilation systems can increase the amount of natural ventilation via a) open windows, doors, or skylight, b) roof ventilators, c) stacks, and d) specially designed inlet or outlet openings. Opening windows can help bring in fresh outdoor air and dilute and exhaust contaminants in the indoor air. Natural ventilation through windows can be effective but is dependent on factors that drive pressure differentials between outdoors and indoors, like wind pressure and stack (or buoyancy) effects. Therefore, airflow into the building, even with open windows, is not guaranteed. To help address this, schools can consider using window fans or box fans positioned in open windows to blow fresh outdoor air into the classroom via one window and indoor air out of the classroom via another window. Note that devices that simply recirculate the same indoor air without filtering it or replacing it with fresh air are not helpful in reducing any airborne virus present in the room (including most window air conditioning units, fans used in rooms with closed windows, and fan coils and radiators).
In some cases, it is not reasonable to bring in additional outdoor air. For example, on very hot summer days or very cold winter days it may not be possible to maintain a comfortable temperature in the classroom if the windows are open. Mechanical ventilation systems, similarly, may need to recirculate more indoor air and bring in less fresh outdoor air when extremely hot or cold outdoor air cannot be sufficiently cooled or heated before it is blown into classrooms. Other factors may also impact the ability to increase outdoor air ventilation, particularly for naturally ventilated buildings, including but not limited to, security concerns, high outdoor air pollution or pollen levels, or high outdoor noise levels. The highest tolerable amount of outdoor air ventilation should still be used, even if students, teachers, and administrators have to adjust their clothing to be comfortable (e.g., wear a jacket indoors in the winter). In cases where the outdoor air ventilation rate cannot be increased, the minimum ventilation rates specified by ASHRAE 62.1 should be met while other strategies such as enhanced filtration and air cleaning are used to achieve a combined 4-6 ACH from ventilation and filtration. In the future, schools may consider indirect energy exchangers such as heat recovery ventilators (HRV), energy recovery ventilators (ERV), and desiccant systems to retrieve energy from the conditioned return air but avoid mixing the air.
Filtration in school buildings can help mitigate long-range airborne viral transmission by removing SARS-CoV-2 from air that is mechanically recirculated through the building. In buildings with mechanical ventilation systems, existing filters can be upgraded to filters with efficiency ratings of at least MERV 13 or the highest MERV rating the system can handle based on the pressure drop and system capacities (e.g., fan power). MERV ratings, developed by ASHRAE, indicate the percentage of particles and the sizes of particles that filters can remove from air passing through them. Filters with higher MERV ratings remove higher percentages of particles and more effectively remove small particles than filters with lower MERV ratings. Filters with MERV ratings of 13 or higher are recommended for SARS-CoV-2 by ASHRAE. Filters need to be periodically replaced and inspected to make sure they are sealed and fitted properly, with no gaps or air bypass. In some cases, if the airflow distribution system is not designed to handle a higher MERV filter, air could leak around the filter edges, compromising any benefit that might have even been gained from a lower MERV filter.
Portable air cleaners with high-efficiency particulate air (HEPA) filters may be useful to reduce exposures to airborne droplets and aerosols emitted from infectious individuals in buildings. Portable air cleaners are typically most effective in smaller spaces, and care must be taken when choosing a device to ensure it is the correct size for the room where it will be used. One metric to consider is the clean air delivery rate (CADR). The CADR reflects both the amount of air that a unit can process per unit time and the particle removal efficiency of the filter. A helpful rule of thumb is that for every 250 square feet of space, a CADR of about 100 cubic feet per minute (cfm) is desirable. CADR is not the only factor to consider. Portable air cleaners vary in their ability to circulate air in the room, so not all devices with the same CADR rating are equivalent. Devices that provide better mixing of the indoor air can capture particles from more of the room’s airspace and are therefore preferred. Because potential viral sources could be in various locations within a room, it may be beneficial to have several units that meet the target CADR values rather than a single larger unit. For example, if a room needs 300 cfm provided by air cleaning, placing two portable air cleaners with CADRs of 150 cfm or three portable air cleaners with CADRs of 100 cfm, in different locations of the room, may be more effective than using just one portable air cleaner with CADR of 300 cfm. In larger spaces, industrial-sized supplemental ventilation and filtration units are available and should be considered. Furthermore, room airflow patterns and the distribution of people in the room should be considered when deciding on air cleaner placement that maximizes source control and prevents airflow from crossing people. Since air cleaners should be operated while people are present, it may be important to compare different models to find one that does not generate disruptive noise. Reviewing the decibel or sound ratings, which are available for some devices, and selecting a lower value can help identify a quieter option.
Mechanical HVAC systems in buildings tend to get out of tune. Within several years of construction, ventilation airflows may change from how they were designed. Schools can ensure that there is adequate ventilation and filtration through a process of commissioning and testing. Commissioning is the process of checking HVAC performance to ensure that systems are operating as designed. Commissioning and testing should be performed by trained individuals and should be performed throughout the school year.
In between commissioning events, there are several ways to test whether a classroom’s ventilation delivers sufficient outdoor air. In addition to working with trained experts, a school could quickly evaluate ventilation performance using carbon dioxide (CO2) as a proxy for ventilation using low-cost indoor air quality monitors. In an unoccupied classroom, background CO2 would be approximately equal to the concentration of CO2 in the atmosphere: 410 ppm. When students and teachers are present in a classroom, they exhale CO2 into classroom air at a relatively constant rate causing CO2 to rise above the background concentration. At some point, the concentration of CO2 reaches an equilibrium based on the amount generated indoors, and the amount diluted by ventilation. This is called ‘steady-state’ and can be used as a quick indicator of ventilation performance. Lower CO2 concentrations while students are present suggest that outdoor air ventilation rates are acceptable; higher CO2 concentrations suggest other strategies are needed. Instructions for using a low-cost CO2 monitor to estimate classroom outdoor air ventilation rates can be found in this 5-step guide to checking ventilation rates in classrooms: https://schools.forhealth.org/ventilation-guide
It is important to note that while CO2 measurements are a good indicator of overall ventilation, they will not indicate whether other air cleaning interventions are effective. For example, if a classroom is operating portable air cleaners to remove the virus from air, viruses and other pollutants will be removed even if CO2 remains high because cleaners with HEPA filters are not designed to remove CO2.
Lower CO2 concentrations while students are present suggest that outdoor air ventilation rates are acceptable; higher CO2 concentrations suggest other strategies are needed.
Additional air quality controls can be considered, including maintaining higher humidity and air cleaning with ultraviolet germicidal irradiation (UVGI). Because these controls require great care in implementation, they are listed in this separate section as advanced considerations. Schools that consider these approaches should consult with outside technical experts.
People’s physiological defenses against respiratory viral infection function best in mid-range humidity levels. Humidity also impacts environmental quality: dry environments are associated with higher incidence of some viral infections, such as influenza, but too much humidity can increase the presence of mites and lead to mold growth. ASHRAE suggests that maintaining relative humidity between 40% and 60% may help reduce COVID-19 infection rates. Note that most buildings cannot easily adjust humidity with existing systems, and that ventilation and filtration should be prioritized. For more information on indoor relative humidity and temperature combination setpoints within this relative humidity range that are aimed at providing a healthy as well as a comfortable environment for occupants, for winter and summer operation, refer to the ASHRAE’s Pandemic Task Force’s reopening plan for schools and universities.
UVGI is an air cleaning technology that is sometimes used in buildings. UVGI uses low-wavelength ultraviolet light (UVC light) to destroy viruses. UVGI has been shown to be effective in disinfecting surfaces and air from bacteria and viruses such as influenza. In buildings, this technology is usually deployed as upper room UVGI to destroy airborne virus in the upper airspace of a room or as UVGI in supply air ducts to destroy airborne virus present in recirculated air. UVGI may be able to reduce exposures to airborne COVID-19. In order for UVGI to be effective, there must be sufficient contact time between the virus and the UV light; this often presents a challenge for installing an effective in-duct UVGI system. Similarly, upper room UVGI works best when the air in a room is well mixed so that airborne virus emitted by people in the lower portion of the room is lofted into the upper airspaces where it can be treated. Other potential issues with UVGI in schools include cost, maintenance, and potential health concerns of inadvertent UV exposures. In general, UVGI should be further discussed with an expert before consideration for use in a school.
Schools that cannot adequately ensure physical distancing might consider installing physical barriers (e.g., plexiglass separators) in select areas. Plexiglass is a clear, solid material that acts to block transmission of large droplets between two people in close contact. Consider installing plexiglass shielding in areas where there is fixed and steady interaction, like the reception desk and cafeteria checkout. Within classrooms, plexiglass shielding may be useful for physically separating students who share tables, and as an additional barrier between the teacher and student areas of the classroom. Installing plexiglass barriers may create areas within a room with uneven mixing of the air. This can inadvertently increase the concentration of airborne SARS-CoV-2 in localized areas. Schools should consider asking experts to check air mixing and interzonal airflows in indoor environments after installing plexiglass barriers to ensure no disruption of ventilation and airflow.
To limit fomite transmission, existing infrastructure could be replaced with contactless alternatives. For example, doors with handles could be replaced with automatic doors. If installing new infrastructure is not feasible, alternative policies could be implemented (e.g., doors could be propped open, so students do not need to touch them).
In addition to infrastructure, technology in bathrooms, classrooms, cafeterias, and other locations should be made as touchless as possible. This includes automatic dispensers of hand soap, hand sanitizer, and paper towels. Contactless hand sanitizer dispensers at the entrance inside classrooms could improve hygiene of students during transitions between activities and after touching shared objects or surfaces within classrooms. Additionally, foot pedals could be installed to replace buttons on water fountains.
Shared equipment, spaces, materials, and surfaces should be cleaned and disinfected throughout the school day. Special attention could be paid to the most highly touched surfaces, such as door handles, light switches, sink handles, and any elevator buttons. In addition to cleaning by janitorial or custodial staff, provide teachers and classroom staff with disinfectant wipes to disinfect items in their classrooms between uses. The infectious virus does become inactivated over time without cleaning, but this would not be acceptable for objects regularly reused or frequently touched surfaces. The EPA has compiled a list of safe and recommended disinfectant products for use against COVID-19.
Remember, frequent hand-washing is the best defense against transmission from contaminated surfaces.
In addition, schools should ensure custodial and janitorial staff have sufficient personal protective equipment to safely clean contaminated areas, including any necessary facemasks, gloves, goggles, and gowns. They should also be trained in proper disinfection protocols and safety practices during cleaning (e.g., washing hands afterward, discarding disposable equipment, opening windows/doors to increase fresh air when possible, staying home when sick), and in best disinfection practices to prevent fomite transmission of COVID-19.
SARS-CoV-2 has been found on toilets and in stool of COVID-19 hospital patients, indicating that bathrooms may be places where elevated fomite and long-range airborne transmission could occur through touching shared surfaces and breathing bioaerosols generated by toilet flushing.
Fomite transmission risk in bathrooms may be minimized by handwashing and installing touchless faucets, soap dispensers, towel dispensers, and doors. In some cases, it may be appropriate for an adult to be present to assist with or monitor handwashing in the bathroom, particularly for small children. It may also be prudent to have children wash their hands with soap and water or use hand sanitizer after they return to their classroom in a location where their teacher can monitor hand hygiene.
Fomite transmission risk in bathrooms may be minimized by handwashing and installing touchless faucets, soap dispensers, towel dispensers, and doors.
In order to prevent the spread of contaminants from bathrooms to other indoor spaces, negative pressure differentials with respect to other building zones should be maintained by running bathroom exhaust fans continuously, and keeping bathroom doors and windows closed at all times, even when not in use. Long-range airborne transmission risk in bathrooms may be further minimized by installing toilet lids, keeping lids closed when not in use, and encouraging students to close the lids before flushing.
Before re-occupying the school building after closures, schools should flush all bathroom faucets, drains, and toilets in case the water in the p-traps has evaporated. In addition, any time there is a sewer gas smell, schools should make sure to fix the plumbing.
Finally, bathrooms can be places where crowding occurs, especially when children have shared windows of time when they can use the bathroom. To enforce physical and group distancing and to minimize crowding, it may be useful to close bathrooms during transition periods and promote bathroom breaks during class time instead, to assign classrooms to use specific bathrooms or to stagger the timing of scheduled bathroom breaks by class.